In a perfect world, you would never need to save your child’s life. But, unfortunately, emergencies are a part of life and they can happen no matter how vigilant and careful you are. No parent wants to be put in that situation, but if you are, you certainly want to know what you’re doing. Babies, while equipped with many reflexes and instincts that give them the best possible chances of survival, are still just babies. They can easily choke on a piece of food or small object that has found its way into their mouths, or get tangled in a long cord hanging from the blinds. Sure, you can do your best to prevent injury by baby-proofing the house and whatnot, but accidents can always still happen. This is especially true as your child gains mobility and you need to become more watchful than ever. The best way you can protect your little one is to learn life-saving techniques so you’re prepared for whatever life throws at you. Even if you’ve been CPR-certified before, one of the best things you can do as a parent is to take a refresher course because the last thing you would want to do is freeze during an emergency.
WHY IS CPR IMPORTANT?
CPR, or cardiopulmonary resuscitation, is an emergency lifesaving procedure performed when the heart stops beating. When the heart stops beating properly, the lungs cannot get new oxygen into the body, and cells and tissues begin to die. Certain types of cells can only survive 4-6 minutes without re-oxygenation, and this includes brain cells. This means that after 10 minutes of not breathing, many brain cells have died and a person is unlikely to recover from the damage. CPR provides emergency care to a victim whose heart and lungs are not working properly until paramedics can come and take over.
SHOULD I CALL 911 FIRST OR INITIATE CARE?
Ideally, you would begin CPR immediately while a second person at the scene calls 911. It takes an ambulance approximately 8 minutes to arrive, but the time increases in rural areas, so beginning CPR right away is crucial. However, in the case that you are alone, follow the rules below.
Call 911 first for:
- any person 12 years or older who is unresponsive
- a child or an infant whom you witnessed suddenly collapse
*Ideally, you will call 911 on speaker phone while you attend to the victim
Initiate care first for:
- an unresponsive infant or child younger than 12 years whom you did not see collapse
- a person who is choking (since they’re not unresponsive. You want to tend to them first)
- a person who is experiencing a severe allergic reaction and has an EpiPen (epinephrine auto injector)
- a person who has severe, life threatening bleeding
HOW TO PERFORM CPR ON AN ADULT OR A CHILD:
- Assess that the scene is safe. Is there poisonous gas, electrical wires, an active shooter, etc.? Blindly entering the emergency situation without assessing your environment can put your life in danger too.
- Tap the collar bone of the victim and shout, “Are you okay?” If the victim is not breathing or responding, you can assume that cardiac arrest has occurred. If the victim is unresponsive, consent is implied. If the victim is a minor and the parent or guardian is present and responsive, you must gain consent. If the victim is not responding, yell for help and have someone call 911 and get an AED.
- Begin chest compressions as soon as possible. Done correctly, chest compressions generate blood flow to vital organs. Perform a minimum of 100 chest compressions a minute and a maximum of 120 per minute. Perform chest compressions with the right depth of about 2-2.4 inches for an adult and about 2 inches for a child. This is a third of the depth of the chest. Allow the chest to fully recoil after each compression. Avoid interruptions between compressions.
- Administer 2 breaths after every 30 compressions. After the first set of 30 compressions, open up the airway using a head tilt and chin lift on the victim and give 2 breaths.
- Mouth-to-mouth: give 1 breath for 1 second, then take a regular breath, and give a second breath for another second. Pinch the victim’s nose when giving breaths.
- Mouth-to-nose: if breaths through the mouth are impossible because the mouth can’t be opened, you can give breaths around the nose. Close the mouth when giving breaths through the nose.
- Giving too much air can cause gastric inflation and increase the chances of the victim throwing up, so avoid excessive breaths. You are only trying to make the chest rise.
HAND POSITIONING FOR A CHILD OR ADULT
Place the heel of one hand on the center of the victim’s chest and the heel of the other hand on top of the first hand so that the hands are overlapped and parallel. Interlock the top hand’s fingers into the bottom hand.
Two handed chest compressions is the most common technique for adults and children, but for children aged 1-8 years, a one-handed technique can be used to achieve the proper depth.
*Things to consider:

HOW TO PERFORM CPR ON AN INFANT (YOUNGER THAN 12 MONTHS)
- Assess the scene.
- Gain consent from a parent or guardian (if not yourself).
- Tap the bottoms of the feet while securing the head, and shout, “Are you okay?”
- Check for breathing, but do not check longer than 10 seconds. If the infant is not breathing, call 911.
- Before beginning CPR with compressions, make sure they are laying on a hard surface. Perform a minimum of 100 chest compressions a minute and a maximum of 120 compressions per minute. The right depth for an infant is about 1.5 inches. Use two fingers with the knuckles stacked on top of each other to perform compressions. Infants need less pressure, as the cartilage is much softer.
- After delivering 30 chest compressions, issue 2 rescue breaths. While supporting the forehead, position the infant’s head into a slight “sniffing” position, which is a very slight tilt. Infants’ airways are small, so positioning the head too far back can actually restrict the airway. Cover the infant’s mouth and nose with your mouth and deliver two, 1 second breaths while looking for chest rise and fall. Do not over inflate the lungs as this can force air into the stomach and cause vomiting.
- Continue CPR with cycles of 30 chest compressions, followed by 2 breaths, until paramedics or an AED arrives.

WHAT IS AN AED?
AED stands for automated external defibrillator and is a medical device designed to analyze the heart’s rhythm. Once an AED arrives on the scene, open it, turn it on, and follow the voice prompts. After analyzing the heart rhythm, it will advise whether or not to deliver a defibrillation or electrical shock.The AEDs shock helps regulate the heart rhythm, and if someone is in cardiac arrest, the only effective way for them to regain a regular heart rhythm is through the use of an AED.
AED USE ON ADULTS AND CHILDREN OVER 55LBS:
If an AED is available, you want to use it, but it is crucial that you do not use pediatric pads or pediatric AED settings on an adult as they will not deliver a strong enough defibrillation. Adult pads should be used on children over 55lbs.
- Turn on the AED and follow the voice prompts.
- Use scissors to remove all clothing covering the chest, including a bra. If there is excessive chest hair and the pads cannot attach properly, it may be necessary to shave the area quickly. If there is water pooled on the chest, wipe it off.
- Place one pad (as indicated on the pad itself) on the upper right side of the chest and the other on the lower left side of the chest below the armpit. It is important that the pads do not touch each other.
- Plug the connector cable into the AED if it is not already attached. Allow the AED to analyze for shock by making sure everyone is clear from the body.
- With everyone clear out of the way, deliver a shock if the AED prompts you to. After the shock is delivered, return to CPR with compressions unless advised not to do so.
- Continue giving CPR and follow AED’s instructions until there is an obvious sign of life or paramedics arrive.
*Things to consider:
AED USE ON INFANTS & CHILDREN UNDER 55LBS
- Turn on the AED and follow voice prompts.
- Use scissors to remove all clothing covering the chest. If there is water pooled on the chest, wipe it off.
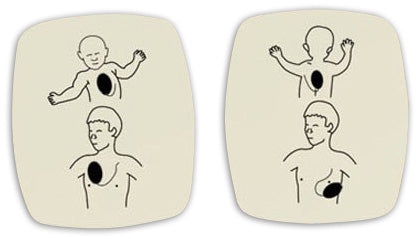
- Using the pediatric pads, place one pad (as indicated on the pad itself) on the middle of the chest and the other on the infant’s back while supporting the head when turning them over.
- Plug the connector cable into the AED if not already attached. Allow the AED to analyze for shock by making sure everyone is clear from the body.
- Deliver a shock if the AED prompts you to. After the shock, promptly return to CPR with compressions, unless advised not to do so.
- Continue giving CPR and follow the AEDs instructions until there is an obvious sign of life or paramedics arrive.
WHAT TO DO IF A CHILD OR ADULT IS CHOKING:
- Deliver 5 back blows followed by 5 abdominal thrusts in rapid sequence until the obstruction is relieved. Before giving care, obtain consent by asking if you can help. They can nod as a confirmation.
- If the victim becomes unresponsive, slide the victim to the floor and call 911.
- Begin CPR with chest compressions right away. After 30 compressions, open the airway to check if you see the object so you can remove it. Do not stick your fingers in the mouth or throat searching because you might push the object further down or injure the victim.
- Try to give 2 breaths and continue with cycles of 30 chest compressions, checking the airway and attempting breaths, until the object is removed or until paramedics arrive.
WHAT TO DO IF AN INFANT IS CHOKING:
- Obtain consent if the parent is present.
- Support the infant’s face and place them face down on your arm.
- Issue 5 back blows between the shoulder blades.
- Rotate the infant over to their back while supporting the head and issue 5 chest thrusts in the same location as CPR, but with the infant at a 45 degree angle towards the floor. These thrusts push air in the opposite direction and move the object upwards and out the airway.
- Continue the cycle of 5 back blows followed by 5 chest thrusts until the victim becomes unresponsive or the object is removed.
- If the victim becomes unresponsive, gently lower them to the ground.
- Call 911 immediately and begin performing CPR with 30 chest compressions, followed by 2 breaths, checking to see if the object has become dislodged each cycle before the breaths.
- Continue CPR until the infant regains consciousness or paramedics arrive.































